

Tooth extraction is a carefully considered treatment, not a first resort. Our goal is always to preserve natural teeth when possible, but there are situations where removal is the safest path to protect a patient’s oral and overall health. When extraction is recommended, the decision is based on a thorough assessment of the tooth’s condition, the surrounding bone and gum health, and how the tooth affects neighboring teeth and bite function.
Patients can expect a clear explanation of why removal is the most appropriate option, what the procedure will involve, and the alternatives that were considered. We place a strong emphasis on patient comfort and clear communication so you understand the clinical reasons behind any recommendation. When appropriate, we discuss replacement options as part of a long-term plan to restore function and appearance.
Corona Family Dental supports patients at every step — from diagnosis and planning through recovery and restoration. Our approach balances clinical expertise with practical guidance so that patients can make informed decisions about their care.
Primary (baby) teeth that interfere with normal development
Sometimes a baby tooth retains its position too long or becomes fused to the jawbone, which can block the eruption of the permanent tooth. In these cases, removing the retained tooth helps guide the permanent tooth into place and prevents alignment problems that might require more extensive treatment later.
Permanent teeth with irreparable decay or structural damage
When decay or trauma destroys most of the tooth’s structure, restoration may no longer be viable. Extracting a non-restorable tooth prevents ongoing infection and pain and allows the dental team to plan for replacement options that restore chewing ability and maintain the integrity of the bite.
Severely fractured or split teeth
Cracks and fractures vary widely in severity. If a crack extends into the root or the fracture leaves insufficient tooth to support a crown or other restoration, removal may be the most predictable treatment. Early evaluation helps determine whether a tooth can be saved or whether extraction is the safer long-term choice.
Advanced periodontal disease that compromises support
When periodontal disease has destroyed the tissues and bone that anchor a tooth, the tooth can become loose and symptomatic. Removing teeth that no longer have adequate support can reduce infection risk and help stabilize the remaining dentition.
Impacted or problematic wisdom teeth
Third molars often lack room to erupt properly and can contribute to pain, decay, or damage to adjacent teeth. In many patients, removing one or more wisdom teeth prevents future complications and preserves the health of surrounding structures.
Extractions to support orthodontic treatment
Orthodontic goals sometimes require creating space to move teeth into ideal positions. Selective extraction of permanent teeth can be an essential part of a coordinated orthodontic plan to achieve a stable, functional, and esthetic result.
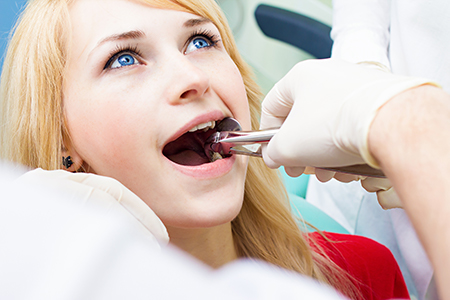
Preparation begins with a detailed review of your medical and dental history. Knowing current medications, systemic health conditions, and previous surgical experiences allows the dentist to tailor the plan and reduce risks. Patients should tell us about any recent illnesses, prescriptions, or over-the-counter medications they are taking so we can advise appropriately.
Diagnostic imaging plays an important role in treatment planning. We use digital radiographs to evaluate root form, proximity to vital structures, and the amount of surrounding bone. These images help determine whether a simple removal is possible or whether a surgical approach will be required.
We discuss comfort measures and anesthesia options before the procedure. Local numbing is standard for most extractions, and for anxious patients or more complex cases we review sedation choices. Clear pre-operative instructions are provided so patients arrive prepared and informed.
A simple extraction applies to a tooth that is visible in the mouth and has an accessible, uncomplicated root structure. After administering local anesthetic to ensure the area is numb, the clinician gently loosens the tooth and uses specialized instruments to remove it with minimal manipulation of surrounding tissues. The procedure is typically quick and well tolerated.
Care during a simple extraction focuses on minimizing trauma to gums and bone and on controlling bleeding. Because the process is less invasive, recovery tends to be faster and discomfort easier to manage with standard pain control measures and short-term activity modifications.
Surgical extractions are required when a tooth is broken at the gumline, impacted beneath bone, ankylosed (fused to bone), or has an unusual root anatomy. These cases may involve a small incision, removal of a portion of bone, and sometimes sectioning the tooth for safer removal. For particularly complex cases, referral to an oral and maxillofacial surgeon may be recommended.
As with all procedures, local anesthesia is provided, and sedation options can be discussed for added comfort. Surgical extractions are performed with attention to tissue preservation to promote predictable healing and to facilitate any planned restorative work afterward.
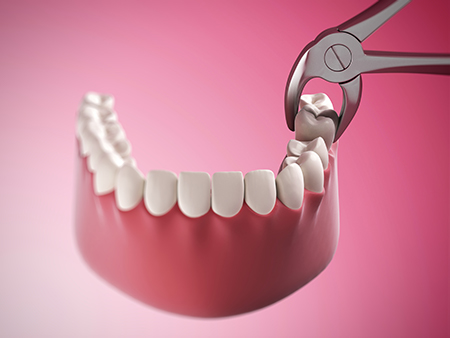
Recovering from an extraction is much simpler when patients follow clear, practical guidance. After the procedure, a gauze pad is typically placed over the site to help a blood clot form. Biting gently on the gauze and keeping steady pressure for the first hour is an important first step. Minor oozing for up to 24 hours is common, but sustained heavy bleeding should be reported.
Patients should protect numb tissues from accidental injury until sensation returns and avoid actions that can disturb a forming clot—this includes rinsing vigorously, using a straw, or smoking in the first 48–72 hours. These habits can dislodge the clot and delay healing. Cold packs applied intermittently on day one can reduce swelling, and a soft-food diet supports comfort while chewing is limited.
Medications may be prescribed to manage pain and, when indicated, to prevent infection. If antibiotics are given, it’s important to complete the prescribed course. Over-the-counter pain relievers can be effective for most patients; use prescription pain medication only as directed.
Use gauze as instructed
Sustained, gentle pressure helps stabilize the initial clot. Replace the gauze only when instructed, and avoid excessive spitting.
Protect numb areas
Don’t chew or touch lips, cheeks, or tongue while anesthesia is active to avoid accidental injury.
Follow medication directions
Antibiotics:
If prescribed, take the full course as directed to reduce infection risk.
Pain control:
Take recommended analgesics before numbness subsides if advised, and follow dosing instructions carefully.
Protect the clot
Avoid rinsing vigorously, drinking through straws, or any activity that creates negative pressure in the mouth during the first few days.
Manage swelling
Apply cold packs intermittently on day one and switch to warm compresses after 48 hours if needed to encourage circulation and comfort.
Skip smoking and tobacco
Avoid tobacco products for at least one week; smoking delays healing and raises the risk of complications.
Choose gentle foods
Stick with soft, cool or warm (not hot) foods and hydrate well. Avoid crunchy, spicy, or carbonated items in the first few days.
Maintain cautious oral hygiene
Brush carefully and use a mild saltwater rinse after 24 hours to keep the area clean—avoid forceful swishing.
Attend follow-up visits
If sutures were placed or the case required additional monitoring, keep scheduled appointments so the team can confirm healthy healing.
If you experience increasing pain, persistent swelling, fever, or any unusual symptoms, contact our office for guidance and timely assessment.
Removing a tooth is often the first step in a coordinated plan to restore chewing function and esthetics. When appropriate, we discuss a range of replacement choices so patients understand how each option affects comfort, speech, and long-term oral health. Common pathways include removable dentures, fixed bridges, and dental implants.
Dental implants are a durable solution that can preserve bone and provide a stable foundation for crowns or bridges, while bridges are often indicated when adjacent teeth can support the restoration. Removable solutions remain valuable for certain clinical situations and patient preferences. We evaluate each patient’s overall health, bone levels, and long-term goals before recommending a restorative plan.
Our team works with you to time restorative treatment appropriately so healing is complete before the next phase begins. Whether you need a straightforward replacement or a more complex restorative approach, the plan will be personalized to restore function and confidence.
Extractions are a routine but significant dental service that can protect oral health and set the stage for long-term, functional restoration. With careful planning, attentive technique, and clear aftercare instructions, most patients recover quickly and move on to appropriate replacement options that restore comfort and appearance. Our team emphasizes safety, transparency, and patient comfort throughout the process.
If you have questions about tooth removal, preventive alternatives, or replacement choices, please contact us for more information. We can review your situation, explain recommended next steps, and help you feel confident about the care ahead.
Tooth extraction is recommended when keeping the tooth would harm your oral health or when the tooth cannot be predictably restored. Common reasons include severe decay or structural damage, advanced periodontal disease that compromises support, irreparable fractures, impacted wisdom teeth, or primary teeth that interfere with normal development. Dentists also consider extractions to support orthodontic plans when creating space is necessary for a stable bite.
Any recommendation for removal follows a careful clinical evaluation that includes a review of your medical history and diagnostic imaging. Your dentist will explain the reasons extraction is the best option, discuss alternatives when appropriate, and outline potential replacement pathways so you understand the next steps in your care.
A simple extraction applies to a tooth that is fully visible in the mouth with an accessible root structure and can usually be removed with elevators and forceps after local anesthesia. These procedures are generally quick, involve minimal manipulation of the surrounding tissues, and tend to have a shorter recovery period. Patients may feel pressure during the procedure but should not experience pain once the area is properly numb.
Surgical extractions are more complex and are required when a tooth is broken at the gumline, impacted beneath bone, fused to bone, or has an unusual root anatomy. Surgical approaches can involve a small incision, removal of bone, or sectioning the tooth for safe removal, and they may require additional sutures and a longer healing period. In especially complex cases, referral to an oral and maxillofacial surgeon may be recommended to manage risk and achieve the best outcome.
Preparation starts with a thorough review of your medical and dental history so the dental team understands any conditions or medications that could affect treatment. Tell your dentist about blood thinners, recent illnesses, allergies, or prior reactions to anesthesia, and follow any specific preoperative instructions such as fasting if sedation will be used. Planning ahead also means arranging transportation home if you will receive sedation and asking questions about the procedure and recovery expectations.
Diagnostic imaging, such as digital radiographs, is often used to evaluate root form and proximity to vital structures, which helps determine whether a simple or surgical approach is necessary. Your dentist will discuss anesthesia and comfort options, provide clear preoperative instructions, and confirm any steps you should take to support a safe, predictable procedure.
Local anesthetic is the standard option for most extractions and reliably numbs the treatment area so you remain comfortable during the procedure. For patients who experience dental anxiety or for more complex surgical cases, additional options such as nitrous oxide (laughing gas), oral conscious sedation, or intravenous sedation can be discussed to increase relaxation and reduce awareness during treatment. The choice of sedation depends on the complexity of the extraction, your medical history, and your comfort preferences.
Before recommending sedation, the dental team reviews your health history and explains expectations, necessary fasting, and post-procedure precautions, including the need for a responsible adult to drive you home if deeper sedation is used. All sedation options are provided with appropriate monitoring and safety measures to minimize risk and maximize patient comfort.
On the day of the procedure you will be seated comfortably, and the clinician will confirm your medical history, obtain consent, and administer the selected anesthesia to numb the area. For a simple extraction the dentist gently loosens the tooth and removes it with forceps; for surgical cases an incision, minimal bone removal, or tooth sectioning may be required to access and remove the tooth safely. Throughout the procedure the team monitors your comfort and takes steps to preserve surrounding tissues for predictable healing.
After the tooth is removed the clinician typically places gauze over the site to help a clot form and may place sutures if needed to support healing. You will spend a short time in recovery where post-operative instructions are reviewed, including how to manage bleeding, swelling, and medication, and when to schedule any follow-up appointments.
Immediately after the extraction, bite gently on sterile gauze to help a stable blood clot form, and avoid disturbing the area by not rinsing vigorously, using a straw, or smoking for at least 48 to 72 hours. Apply cold packs intermittently on the first day to reduce swelling and eat soft, nonabrasive foods while avoiding hot or spicy items that can irritate the site. Protect numb areas to prevent accidental biting of the cheeks, lips, or tongue until sensation returns.
Follow medication directions carefully, taking prescribed antibiotics for the full course if given and using recommended analgesics to maintain comfort—avoid routine use of prescription pain medication beyond the prescribed guidance. Maintain gentle oral hygiene, resuming careful brushing and using a mild saltwater rinse after 24 hours to keep the area clean, and return for scheduled follow-up so the team can confirm proper healing.
The initial healing phase typically occurs over the first one to two weeks, with the most noticeable symptoms—bleeding, swelling, and discomfort—improving substantially after 48 to 72 hours. Mild to moderate pain that responds to over-the-counter or prescribed analgesics, light oozing, and localized swelling are common during the early recovery period. Stitches, when placed, may dissolve or be removed at a follow-up visit, and daily activities can usually resume within a few days depending on the procedure’s complexity.
Complete bone remodeling and soft tissue maturation take longer, often several months, and the timing for any permanent restorative work depends on how quickly the site heals and whether additional procedures like bone grafting are needed. If recovery deviates from the expected course—such as worsening pain, heavy bleeding, or signs of infection—contact the dental team promptly for assessment.
Complications are uncommon but can include infection, prolonged bleeding, dry socket (a painful loss of the clot), swelling that increases after the initial period, or, rarely, nerve irritation when extractions occur near major nerve pathways. Dry socket typically presents as a severe, worsening pain that radiates from the extraction site and may be accompanied by an unpleasant taste or odor. Most issues can be managed effectively when identified early, so monitoring your symptoms and following post-operative instructions reduces risk.
Contact the office if you experience uncontrolled bleeding beyond 24 hours, progressive swelling after 48 to 72 hours, fever, or sudden, severe pain that does not respond to medication. For urgent concerns you can reach our Bradenton or Sarasota office to request guidance and arrange timely follow-up care with the clinical team at Corona Family Dental.
Treatment to replace a missing tooth is planned according to the site’s healing and your overall health; in many cases clinicians wait until soft tissues have closed and initial bone healing has occurred before placing a definitive restoration. Replacement options commonly include dental implants, fixed bridges, or removable dentures, and each choice carries different clinical prerequisites such as sufficient bone volume, healthy adjacent teeth, and long-term maintenance considerations. Immediate temporary restorations may be used in select situations to preserve esthetics while the site heals.
Dental implants often require a period of healing before the implant is placed or before a crown is attached, and some patients may need bone grafting to build adequate support. Your dentist will evaluate imaging and overall oral health to recommend a personalized restorative timeline that balances predictable outcomes with your functional and aesthetic goals.
Yes, primary (baby) teeth may require extraction when they are retained and block the eruption of permanent teeth, when severe decay or infection threatens a child’s health, or when trauma leaves the tooth non-restorable. Pediatric extractions focus on minimizing discomfort and anxiety through clear explanation, child-friendly behavior management, and appropriate use of local anesthesia or mild sedation when necessary. The goal is to protect developing permanent teeth and to guide healthy eruption patterns.
When a primary tooth is removed prematurely, the dental team may recommend a space maintainer to preserve room for the permanent tooth and prevent unwanted shifting. Follow-up care includes monitoring eruption, reinforcing home hygiene, and coordinating with orthodontic planning when needed so the child’s development proceeds predictably.
Quick Links
Locations