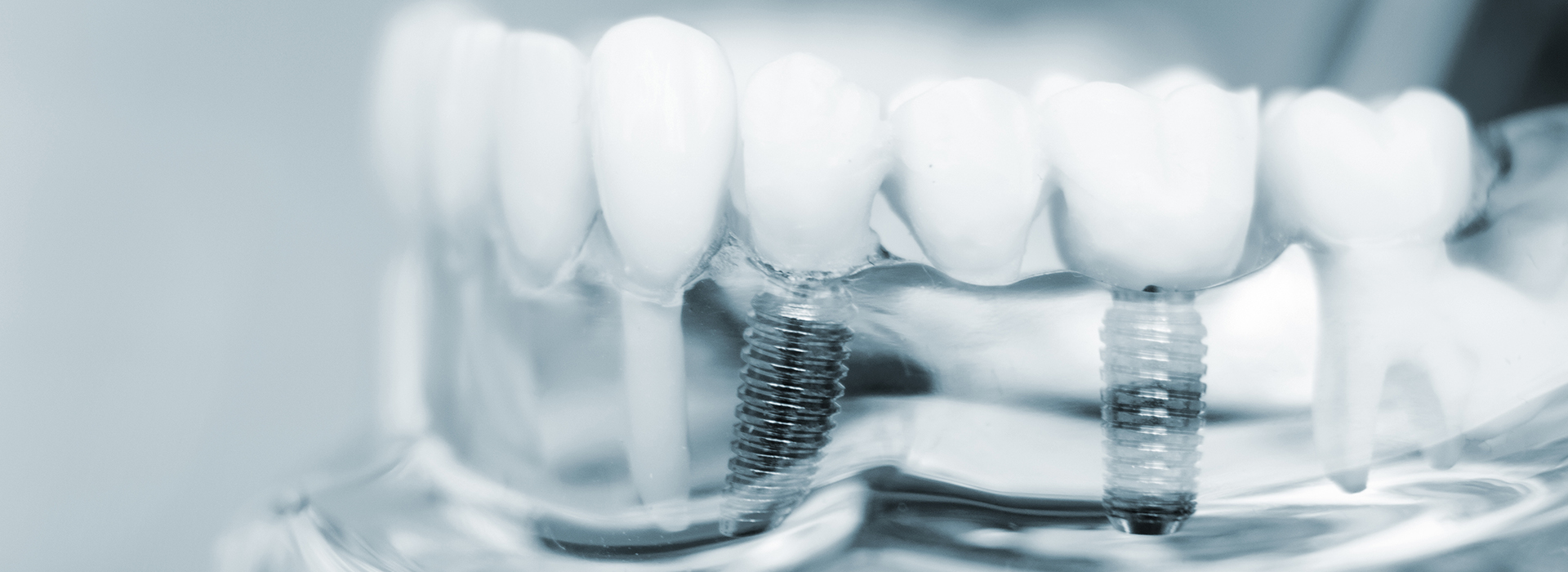

Missing teeth affect more than appearance — they change how you chew, speak, and how your jaw ages over time. Dental implants replace both the visible tooth and its root, giving a level of stability and comfort that closely mimics natural dentition. For many people, implants are the most reliable option for restoring function and preserving long-term oral health.
Implants are made from biocompatible materials that integrate with the jawbone. This integration creates a solid foundation for replacement crowns, bridges, or dentures so the prosthetic behaves much like a natural tooth. Because the implant stimulates the bone, it helps protect facial structure and reduces the progressive bone loss that often follows tooth extraction.
When evaluating tooth replacement options, patients and clinicians weigh durability, comfort, and preservation of surrounding tissues. Dental implants routinely score highly across all three factors, offering a predictable path to a durable, easy-to-care-for smile. Our approach emphasizes clear explanations and tailored treatment planning to match each patient’s needs and goals.

Unlike removable appliances, implants provide fixed support that reduces movement while eating or speaking. That stability restores confidence in everyday activities and eliminates many of the limitations associated with traditional dentures. Because implants don't rely on neighboring teeth for support, they preserve the integrity of surrounding natural teeth.
Implants also simplify daily care: once the final restoration is placed, routine brushing, flossing, and regular dental checkups are typically all that's needed to maintain good results. Their resistance to decay and tendency to maintain bone volume contribute to their long-term value as a restorative option.
Dental implants combine engineering and biology to deliver a durable tooth replacement. The implant post integrates with bone through a process called osseointegration, creating a level of anchorage that traditional prosthetics can't match. This biological fusion supports chewing forces more naturally and can significantly improve the comfort of a restored bite.
Another key advantage is versatility. Implants are not limited to replacing a single tooth; they can support crowns, multi-unit bridges, and even full-arch prostheses. That flexibility allows clinicians to design solutions that meet a patient’s functional and aesthetic priorities without compromising adjacent teeth when possible.
Finally, implants help protect long-term oral health. By replacing the tooth root's role in stimulating the jawbone, implants reduce the rate of bone resorption that often follows tooth loss. Preserving bone helps maintain the proportions of the face and supports neighboring teeth, contributing to a more stable and healthy mouth over time.
With careful planning and precise placement, implants frequently deliver outcomes that feel and function like natural teeth. Patients often experience improved bite efficiency, restored speech clarity, and greater confidence when smiling. Because implants are integrated into the bone, common issues with slipping or clicking that occur with some removable options are minimized.
Proper maintenance is straightforward. While implants themselves don't decay, the surrounding gum tissue still requires attention to prevent inflammation. Regular professional checkups and attentive home care keep both the implants and natural dentition healthy for the long term.
Implant dentistry has evolved into a suite of solutions designed to match different clinical situations. Selecting the right option depends on how many teeth are missing, the condition of the jawbone, and the patient’s desired outcome. The following implant types highlight the kinds of restorations commonly offered in modern practices.
Successful implant treatment begins with comprehensive planning. We evaluate dental and medical history, examine the oral tissues, and use imaging to map bone volume and anatomical landmarks. This diagnostic phase informs a personalized plan that balances function, appearance, and long-term predictability.
Surgical placement is typically performed as an outpatient procedure under local anesthetic, with sedation options available when appropriate. The implant is positioned into the jawbone with a focus on precise angulation and depth; this careful placement supports both healing and the eventual prosthetic design.
After placement, the implant integrates with the bone over several months. During this period, a temporary restoration may be provided to maintain aesthetics and function. Once osseointegration is complete, the final crown, bridge, or denture is fabricated and attached to achieve the desired appearance and bite.
Clear communication about anesthesia, sedation options, and post-operative care helps patients feel prepared and supported. We provide detailed instructions for recovery, including how to manage discomfort and protect the surgical site. Follow-up visits allow the clinician to monitor healing and to transition smoothly from temporary to final prostheses.
Long-term follow-up includes periodic clinical and radiographic exams to ensure the implant and surrounding tissues remain healthy. Maintaining a routine of professional cleanings and conscientious home care is essential to protect the investment in oral health that implant therapy represents.
Bone quantity and quality are central to implant success. When teeth are lost, the jawbone can shrink over time, which may make implant placement more challenging. In many cases, bone grafting or augmentation techniques can rebuild the necessary volume to support an implant securely.
Bone grafting uses graft material to encourage new bone growth in the deficient area. Depending on the situation, grafting can be performed at the time of extraction, before implant placement, or simultaneously with implant surgery. These procedures enable a broader range of patients to become good implant candidates by creating a stable foundation for long-term integration.
With modern protocols and attentive maintenance, implant survival rates are high. Success depends on careful patient selection, precise surgical technique, and ongoing oral hygiene. Regular dental visits help catch and address any issues early, keeping implants and surrounding tissues healthy for many years.
Replacing teeth with implants restores more than function; it often reinstates the self-assurance people feel when they can smile, speak, and eat without hesitation. When tooth loss has affected nutrition, speech, or social comfort, thoughtfully planned implant therapy can address those concerns comprehensively.
Our team brings a patient-centered approach to implant care, focusing on predictable outcomes and clear communication. If you’re exploring implant therapy and want a thorough assessment, our clinicians can explain the options, review the diagnostic findings, and tailor a plan that reflects your priorities.
At Corona Family Dental, we aim to provide reliable information and thoughtful guidance for patients considering implant dentistry. If you’d like to learn more about how implants might restore your smile, please contact us to discuss your options and schedule a consultation.
Dental implants are medical devices that replace a missing tooth by restoring both the root and the visible crown. A typical implant is a biocompatible titanium or titanium-alloy post that is surgically placed into the jawbone and allowed to integrate with bone tissue. This process of bone bonding, called osseointegration, creates a stable anchor for a prosthetic tooth.
Once osseointegration is complete, a custom crown, bridge, or denture is attached to the implant to restore chewing, speech, and appearance. Because the implant takes over the role of the tooth root, it helps preserve jawbone volume and facial proportions that often decline after tooth loss. The end result is a restoration that closely mimics the function and feel of a natural tooth.
Good candidates typically have healthy gum tissue and sufficient jawbone to support an implant, as well as the ability to maintain regular oral hygiene. Certain medical conditions, smoking and uncontrolled systemic disease can affect candidacy, but many patients can become candidates after medical clearance or preparatory treatments. A thorough evaluation including medical history and diagnostic imaging determines whether implants are appropriate.
Treatment is individualized to balance function, appearance and long-term predictability, and alternative options are discussed when implants are not suitable. At Corona Family Dental, clinicians review imaging and clinical findings to recommend the safest and most effective approach for each patient. When additional procedures such as bone grafting are needed, they are explained clearly so patients understand the next steps.
Treatment time varies depending on the clinical situation, diagnostic findings and whether preparatory procedures are required. Initial consultation and planning typically include exams and imaging, and any necessary bone grafting or extractions can add several months to the timeline. Once the implant is placed, osseointegration commonly requires a healing period of several weeks to a few months before the final restoration is attached.
In some cases clinicians offer immediate provisional teeth at the time of placement to preserve aesthetics and function during healing. Full-arch reconstructions and complex cases may follow staged protocols to optimize outcomes and long-term stability. Regular follow-up appointments monitor healing and guide the transition from temporary to final prostheses.
Implant dentistry includes a range of restorations tailored to the number of missing teeth and the patient’s goals, from single-tooth crowns to full-arch prostheses. A single implant topped with a custom crown replaces an individual tooth without altering adjacent teeth, while implant-supported bridges can replace multiple adjacent teeth using strategically placed implants for support. For patients missing all teeth in an arch, fixed full-arch prostheses anchored by several implants provide a permanent, nonremovable solution.
Implant-retained removable dentures are another option that snap onto implants for improved retention while remaining removable for cleaning. The choice of restoration depends on bone availability, functional demands and aesthetic priorities, and clinicians present the options that best meet those needs. Each restorative type is designed to restore function, preserve bone when possible and offer predictable long-term results.
Bone quantity and quality are critical to implant stability because the implant must integrate securely with the jawbone to withstand chewing forces. When teeth are lost the underlying bone tends to resorb over time, which may limit the sites suitable for implant placement without augmentation. Assessing bone with clinical examination and imaging helps determine whether grafting is necessary to create a stable foundation.
Bone grafting options include socket preservation at the time of extraction, ridge augmentation before implant placement and simultaneous grafting at the time of implant surgery when indicated. Grafts may use autogenous, allogenic, xenogenic or synthetic materials depending on the clinical goal and patient preference. With proper technique and healing time, grafting can restore sufficient volume to support predictable implant integration.
Implant placement is generally performed as an outpatient procedure using local anesthesia, and sedation options are available for patient comfort when appropriate. The surgeon positions the implant post into the jawbone with careful attention to angulation and depth to support the planned restoration, and the surgical site is closed to allow healing. Many patients experience mild swelling and discomfort that are manageable with prescribed or over-the-counter medications and short-term self-care.
Dietary adjustments to softer foods and careful oral hygiene around the surgical site are recommended during early healing to protect the implant. Follow-up visits allow the clinician to monitor integration and to provide any temporary restorations needed for function and appearance. Once healing is verified, the final prosthesis is fabricated and attached to complete the restoration process.
Long-term implant success depends on consistent home care and regular professional maintenance, because surrounding gum tissue remains susceptible to inflammation. Daily brushing with a soft brush, interdental cleaning around the implant and flossing to remove plaque are essential habits to prevent peri-implant disease. Using appropriate interdental brushes or floss recommended by your clinician helps control biofilm in hard-to-reach areas.
Professional checkups and periodic radiographic exams allow your dental team to track tissue health and detect early changes that may require treatment. Avoiding tobacco and managing systemic health factors such as diabetes also supports implant longevity. With diligent hygiene and routine care, implants offer durable function and contribute to sustained oral health.
Yes, a range of anesthesia and sedation options can be employed to enhance comfort during implant treatment based on the complexity of the procedure and the patient’s medical profile. Local anesthesia is typically used to numb the surgical site, and additional options such as nitrous oxide, oral sedatives or intravenous sedation may be available for longer or more involved cases. The choice of sedation is made in consultation with the clinician and takes into account medical history, anxiety level and procedural needs.
Monitoring during sedation follows standard safety protocols and recovery is supervised until the patient is stable to go home with appropriate post-operative instructions. Patients should arrange transportation if moderate or deep sedation is planned and follow pre- and post-operative guidelines to ensure safe recovery. Clear communication about comfort options helps patients feel prepared and supported throughout treatment.
Dental implants preserve jawbone by replacing the tooth root, which helps maintain facial structure and supports neighboring teeth, while traditional bridges and removable dentures do not provide this root-level stimulation. Bridges often require preparation of adjacent healthy teeth to serve as anchors, which can compromise those teeth over time, whereas implants restore a tooth without involving neighboring structures. Removable dentures may offer a noninvasive solution but can accelerate bone resorption and provide less stable chewing function.
Implants generally provide superior chewing efficiency, comfort and long-term tissue preservation when placed and maintained properly. That said, implants require a surgical procedure and consistent oral hygiene, so the best restorative choice depends on each patient’s anatomy, health status and treatment goals. A thorough clinical assessment clarifies which option best balances function, appearance and long-term oral health.
Begin by scheduling a consultation so a clinician can review your medical and dental history, perform an oral examination and obtain diagnostic imaging to assess bone and tissue conditions. During this visit you can discuss your goals, ask about the range of implant-supported restoration options and learn what diagnostic steps and preparatory procedures might be necessary. The clinician will outline a personalized treatment plan and explain the expected sequence of care and follow-up steps.
Bring a list of medications and any relevant medical records to the appointment to help the team evaluate systemic factors that may affect treatment. If supplemental procedures such as grafting or extractions are recommended, the clinician will explain timing and healing expectations so you have a clear roadmap. Our offices in Bradenton and Sarasota can coordinate scheduling and provide guidance on what to expect during each phase of care.
Quick Links
Locations