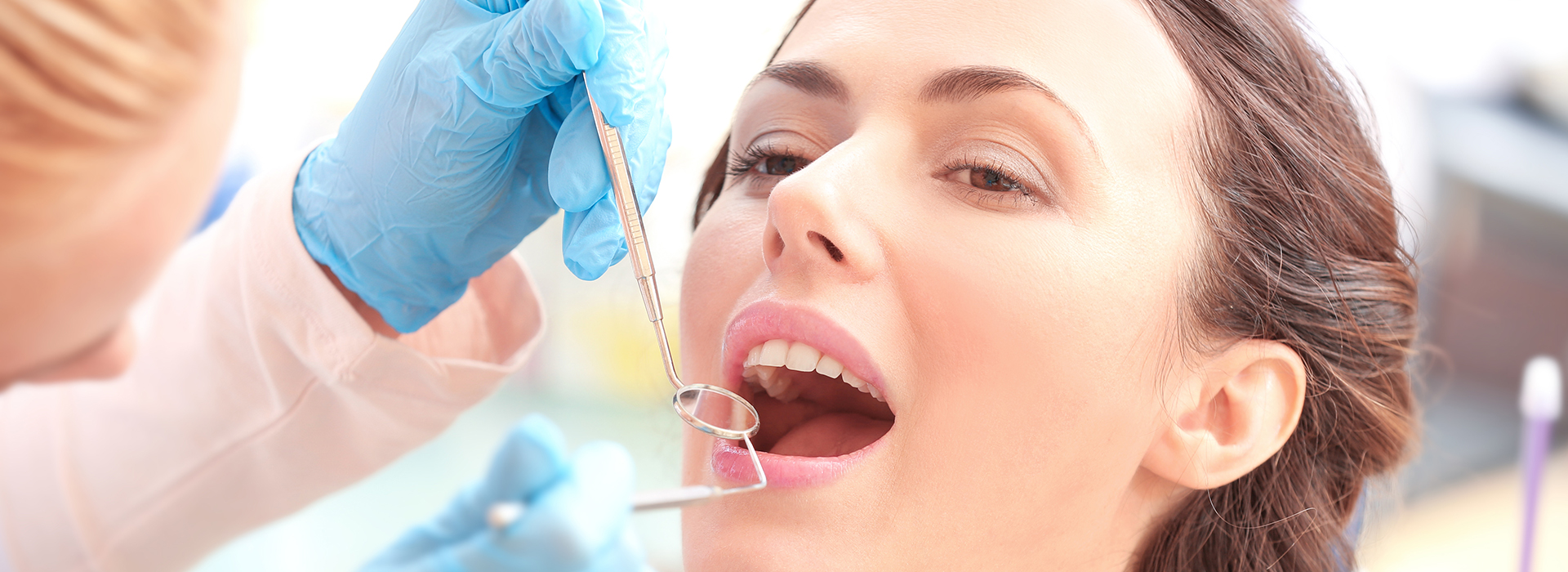

Gum disease is one of the most common—and most overlooked—threats to long-term oral health. Research indicates periodontal conditions affect a large portion of adults, and many cases begin without obvious discomfort. At Corona Family Dental, our goal is to help patients recognize early warning signs, understand how the disease progresses, and access treatments that protect teeth, bone, and overall health. This page explains what gum disease looks like, why it matters, and how modern periodontal care can restore and preserve a healthy smile.
Periodontal disease begins when bacterial plaque accumulates along the gum line and in the small crevices between tooth and gum. Left unchecked, that bacterial film hardens into calculus (tartar), which adheres to tooth surfaces and encourages further inflammation. That inflammation is the body’s response to bacteria—but over time it damages the soft tissues and bone that hold teeth in place.
The earliest stage—often reversible with good home care and professional cleanings—is characterized by inflammation confined to the gums. When the condition advances, pockets develop between the gums and teeth. Those pockets trap more bacteria and create an environment where the infection can progress, sometimes leading to gradual loss of supporting bone and loosening teeth.
Because the initial stages of gum disease can be subtle, routine dental examinations and careful periodontal assessments are essential. Early detection gives you the best chance to stop disease progression with conservative treatments rather than resorting to more invasive measures later on.
Common signs that should prompt an evaluation include:
Gums that appear red, swollen, or tender rather than a healthy pink
Bleeding during brushing or flossing, even if it’s only occasional
Chronic bad breath or a persistent unpleasant taste in the mouth
Notable gum recession, new gaps forming between teeth, or a change in bite
Loose teeth or discomfort when chewing

Healthy periodontal tissue is the foundation for every tooth. Beyond preserving chewing function and appearance, maintaining healthy gums helps protect the jawbone and prevents the cascade of changes that can follow tooth loss—shifting teeth, altered bite, and changes in facial support. Strong periodontal health is central to keeping a natural, functional dentition for life.
Emerging research also highlights links between chronic gum inflammation and systemic health. While the exact connections are complex and still being investigated, long-standing periodontal disease has been associated with conditions such as diabetes, cardiovascular disease, and respiratory issues. Controlling oral inflammation is therefore part of an overall wellness strategy.
Prevention is the most powerful tool: consistent daily cleaning, professional examinations, and targeted periodontal care when needed reduce risk and support whole-body health. Our approach focuses on practical, evidence-based interventions that help patients keep inflammation under control and preserve natural teeth whenever possible.
Gingivitis is the earliest, most treatable stage of gum disease. It occurs when plaque-induced inflammation causes the gums to become red, swollen, and prone to bleeding. Many people dismiss a little bleeding during brushing, but it’s an early signal that attention is required—especially when combined with redness and tenderness.
The encouraging news is that gingivitis is reversible. With improved oral hygiene—thorough brushing twice daily, daily interdental cleaning, and professional dental cleanings—the inflammation usually subsides and the gums return to health. For patients with additional risk factors, such as smoking or certain medical conditions, more frequent monitoring and tailored hygiene strategies may be recommended.
When gingivitis is addressed promptly, permanent damage to the periodontal apparatus can be avoided. Our clinicians provide clear, practical guidance to help patients adopt effective daily routines and use the right tools to keep plaque from reclaiming space along the gum line.

Periodontitis develops when inflammation extends beyond the gum margin and begins to destroy the connective tissues and bone that stabilize teeth. As pockets deepen and bone is lost, the structural support for the tooth weakens. This process is typically slow and progressive, which is why many patients don’t notice it until the disease is well established.
Clinical signs of periodontitis include deep periodontal pockets, receding gums, and increased tooth mobility. Radiographic evaluation often reveals bone loss around affected teeth. Treatment at this stage aims to arrest tissue destruction, reduce pocket depth, and, when possible, rebuild lost structures to improve both function and appearance.
Successful management relies on a combination of mechanical cleaning, targeted use of antimicrobial strategies, and careful maintenance. The objective is to create an environment where the body’s healing processes can stabilize the tissues and where patients can maintain oral health through improved home care and scheduled professional visits.
Treatment plans are individualized to reflect the stage of disease, the extent of tissue damage, the patient’s overall health, and personal goals. Most treatment paths begin with conservative, non-surgical measures designed to reduce bacterial levels and inflammation. When necessary, surgical techniques and regenerative procedures are used to repair and rebuild periodontal support.
Non-surgical periodontal therapy focuses on thorough removal of plaque and calculus from below the gum line and smoothing root surfaces so they are less hospitable to bacteria. These procedures—commonly called scaling and root planing—are typically performed with local anesthesia for comfort and are often complemented by targeted antimicrobial treatments when indicated.
When patients combine these professional measures with consistent home care, many cases stabilize without the need for surgery. The goal is to reduce pocket depth, lower bacterial load, and resolve inflammation so that the tissues can heal and be maintained with routine care.
Our clinicians monitor response to non-surgical therapy and review home-care techniques to ensure patients have the best chance of long-term success. If pockets remain deep or bone loss progresses, additional steps are considered.
When disease has progressed beyond the reach of non-surgical therapy, surgical intervention may be recommended to access root surfaces, reduce pocket depths, and repair damaged tissue. Procedures such as flap surgery allow clinicians to thoroughly debride root surfaces and recontour bone to support healing and easier home care.
Advances in regenerative dentistry mean that lost bone and soft tissue can sometimes be rebuilt using grafts and biologically active materials. These techniques aim to restore the underlying support for teeth, improve stability, and enhance esthetics where recession or tissue loss has altered appearance.
Laser-assisted periodontal therapy may be an adjunct in select cases, helping reduce bacterial burden and promote healing in a minimally invasive way. Treatment choices are discussed openly, with an emphasis on predictable outcomes and maintaining the best long-term oral health.
Periodontal care doesn’t end with active treatment. Ongoing maintenance visits and a committed home-care routine are essential to sustaining improvements and preventing recurrence. Our team works with each patient to design a personalized maintenance plan that fits their health profile and lifestyle.
In summary, periodontal disease is common but manageable when detected early and treated with appropriate, evidence-based care. From reversing gingivitis to stabilizing periodontitis and rebuilding lost support, today’s periodontal therapies offer effective pathways to preserve teeth, improve oral function, and support overall health. Contact us to learn more about periodontal treatment options and how we can help you protect your smile.
Gum disease starts when bacterial plaque builds up along the gum line and between teeth, creating chronic irritation. If plaque is not removed, it mineralizes into calculus that anchors bacteria close to the tissues and makes cleaning more difficult. Individual risk factors such as smoking, uncontrolled diabetes, certain medications, and genetic susceptibility increase the chance plaque will trigger destructive inflammation. Poor oral hygiene and irregular professional care allow the condition to progress from reversible inflammation to more serious disease.
The body’s immune response to bacteria causes the inflammation that damages soft tissue and bone over time. Early gingivitis affects only the gum margin and is often reversible, while periodontitis involves deeper pockets and bone loss that can threaten tooth stability. Identifying and modifying risk factors combined with professional treatment are essential to halt progression.
Common early signs include gums that are red, swollen, tender, or that bleed during brushing and flossing. Persistent bad breath or a sour taste may signal an active bacterial infection in the pockets around teeth. As disease advances, patients can notice gum recession, visible gaps between teeth, a change in bite, or teeth that feel loose. Because some changes occur slowly, routine periodontal assessments are important even when symptoms are mild.
If you observe any of these signs, it is important to schedule an evaluation so measurements and diagnostic imaging can determine the stage of disease. Early detection allows for conservative treatments that are more predictable and less invasive. Delaying care increases the likelihood that surgical intervention will be necessary later on.
Diagnosis begins with a comprehensive clinical exam that includes periodontal probing to measure pocket depths and assess attachment levels. The clinician will look for inflammation, recession, bleeding on probing, and tooth mobility while reviewing your oral hygiene habits. Intraoral radiographs are used to evaluate bone levels and detect patterns of bone loss that may not be apparent on exam alone. Medical history, smoking status, and other risk factors are recorded because they influence both diagnosis and treatment planning.
At Corona Family Dental, clinicians combine clinical measurements and radiographic findings to stage disease and recommend a tailored care plan that begins with the least invasive effective options. This approach ensures that patients receive appropriate monitoring and treatment based on their individual needs. When specialized procedures are required, the team will explain the options and expected outcomes in clear terms.
Non-surgical periodontal therapy typically starts with scaling and root planing, a deep cleaning that removes plaque and calculus from below the gum line and smooths root surfaces. These procedures are often performed under local anesthesia to maximize comfort and allow thorough debridement. Adjunctive measures may include localized antimicrobial agents, medicated rinses, and short-term systemic antibiotics when indicated.
When combined with improved home care, non-surgical therapy can reduce pocket depths and resolve inflammation in many cases. The clinical team will reassess healing after therapy to determine whether further treatment or maintenance is necessary. Regular periodontal maintenance visits are a key component of long-term success following non-surgical care.
Surgical treatment is considered when pockets remain deep after non-surgical therapy or when anatomy prevents adequate access for cleaning. Other indications include areas of progressive bone loss, persistent infection, and defects that compromise tooth stability. Surgery allows clinicians to visualize and clean root surfaces directly and to reshape bone to facilitate healing and future maintenance.
Surgical approaches range from flap procedures that reduce pocket depth to bone recontouring and tooth-sparing surgeries designed to preserve function. In some cases, regenerative techniques are combined with surgery to promote new bone and tissue growth in localized defects. The decision to operate is based on diagnostic findings, patient health, and long-term prognosis for the affected teeth. The team will discuss expected outcomes, recovery, and follow-up care before moving forward.
Regenerative periodontal procedures use bone grafts, barrier membranes, and biologically active materials to encourage the body to rebuild lost bone and connective tissue. These techniques are aimed at restoring the structural support around teeth and improving stability and esthetics in areas of tissue loss. Success depends on defect type, patient health, and strict adherence to post-operative care instructions.
Not every case is a candidate for regeneration, but when appropriate these procedures can improve long-term tooth retention and function. Patients who smoke or have uncontrolled systemic conditions may have reduced healing potential and will receive counseling on optimizing outcomes. Careful case selection and maintenance are essential to maximize the benefits of regenerative therapy.
During scaling and root planing your provider will numb the area with local anesthesia and use specialized instruments or ultrasonic devices to remove plaque and calculus from root surfaces. The goal is to disrupt bacterial colonies and create a cleaner root surface that supports healing. Procedures may be completed in one or several visits depending on the extent of treatment and patient comfort.
After treatment you can expect some sensitivity, mild swelling, and occasional bleeding that usually subsides within a few days to a couple of weeks. Your clinician will provide home-care instructions, recommend temporary dietary modifications if needed, and schedule follow-up visits to monitor healing. Adhering to recommended oral hygiene practices and periodontal maintenance appointments improves the chance of long-term stabilization.
Frequency of periodontal maintenance is individualized based on disease severity, response to treatment, and risk factors such as smoking or systemic illness. Many patients benefit from recall visits every three months after active therapy, while others with mild disease may be maintained at longer intervals. These visits typically include careful evaluation, targeted cleaning below the gum line, and reinforcement of home-care techniques.
Consistent maintenance is the single most important strategy to prevent recurrence and preserve results achieved during active treatment. The clinician will adjust the interval over time based on clinical findings and long-term stability. Keeping scheduled maintenance appointments and practicing daily plaque control are essential for protecting periodontal health.
Chronic periodontal inflammation has been associated with systemic conditions such as diabetes and cardiovascular disease, and it may influence overall inflammatory burden. While research continues to clarify causal links, managing oral inflammation is a recognized component of comprehensive health care. Clinicians consider medical history and coordinate with medical providers when systemic conditions might affect periodontal treatment or healing.
Controlling gum disease can help improve glycemic control in some patients with diabetes and may reduce inflammatory markers that impact general health. Patients with complex medical conditions should share their health information so treatment plans can be tailored safely and effectively. A collaborative approach between dental and medical teams supports better outcomes for patients with interconnected health concerns.
To schedule an evaluation call or request an appointment with our Bradenton or Sarasota offices; the team will gather a brief medical history and explain the diagnostic steps we will take. During the visit you can expect a clinical exam, periodontal probing, and radiographs if needed to assess bone levels and tissue health. Knowing what to expect ahead of time reduces anxiety and helps ensure an efficient assessment.
Bring a list of current medications, a summary of your medical history, and any recent dental records or X-rays if you have them available. Prepare a short list of symptoms, questions, and your daily oral hygiene routine so the clinician can offer personalized guidance. If you are a current patient of Corona Family Dental, bring any prior treatment notes or recall information to help the team plan your care.
Quick Links
Locations